All published articles of this journal are available on ScienceDirect.
Arthroscopic Standard Anterior and Posteromedial Portal Posterior Cruciate Ligament Reconstruction With Remnant Preservation: 2-Year Follow-up
Abstract
Background:
Grade 3 Posterior Cruciate Ligament (PCL) injury needs surgical intervention, but there is no consensus on the optimal technique in PCL reconstruction. The old technique always removes the remnant for good visualization of tunnel replacement. Recently, many studies proposed the concept of the preservation of PCL remnant with achieving good visualization. The aim of the study is to evaluate PCL reconstruction with remnant preservation using the standard anterior and posteromedial portal at 2-years follow-up.
Methods:
We conducted a cohort retrospective study between January 2013 to December 2015. In this study, 25 patients underwent PCL reconstruction using standard anterior and posteromedial portal with remnant preservation. We used quadrupled hamstring autograft. The patients were assessed using the International Knee Documentation Committee (IKDC) score, Lysholm knee score, Modified Cincinnati Score, and Knee Society Score (KSS) at pre-operative and 2-years post-operative. Range of Motion (ROM) and complication were evaluated post-operatively.
Results:
The mean diameter of the quadruple hamstring graft was 8 mm. Clinical outcomes enhanced significantly (p<0.05). The average Lysholm activity scale improved from 65.12 ± 10.48 to 94.96 ± 4.80. The International Knee Documentation Committee (IKDC) score improved from 60.50 ± 15.10 to 95.60 ± 3.44. The Modified Cincinnati Score improved from 62. 28 ± 13.6 to 96,04 ± 1.62. The KSS also improved from 60.12 ± 18.01 to 94.88 ± 6.36. 22 patients had 0-135° full ROM and 3 patients had 0-110° ROM. Two patients had surgical site infection but recovered with local debridement.
Conclusion:
PCL reconstruction using standard anterior and posteromedial portal with remnant preservation at 2 years follow up resulted in satisfactory clinical and functional outcomes.
1. INTRODUCTION
Posterior Cruciate Ligament (PCL) reconstruction indicates in grade 3 PCL rupture, avulsion fracture of PCL, combined ligamentous damage associated with the PCL, chronic injuries with persistent instability, or pain despite nonsurgical treatment. PCL reconstruction studies enhance anatomical and biomechanical knowledge of PCL. There are many types in PCL reconstruction such as single bundle, double bundle, transtibial, and tibial in-lay procedures. The surgeon can use only anterior portal, anterior and trans-septal portal, and anterior and anterolateral portal in the PCL reconstruction procedure. However, there is no consensus about the best and most recommended technique in PCL reconstruction [1-7].
PCL injury usually preserves both femoral and tibial insertion at PCL and menisco-femoral ligament [4]. During PCL reconstruction, the remnant fibers are generally removed to obtain full visualization of the original ligament attachment site. It can help the surgeon to create an accurate tibial tunnel for maintaining anatomical and biomechanical of reconstructed PCL like native PCL [1, 4, 8]. PCL had mechano-receptors located at the femoral and tibial attachments and also on the surface of the ligament. These neural networks play an important role in regulating the contraction of muscle groups that give proprioceptive input for maintaining knee stability [4, 9]. PCL remnant may provide biomechanical knee stability and rapid neovascularization for grafted tendons. PCL reconstruction with remnant preservation technique may contribute to post-operative knee stability, graft healing, and proprioceptive function [1-4]. Some surgeons used various techniques from adding arthroscope 70o, anterior and posterolateral portal, and also transeptal portal to achieve good visualization for tunneling [1, 10]. In this study, we used a simple technique with anterior and posteromedial portal for good visualization and preserve the remnant PCL.
The purpose of this study is to evaluate the functional outcome after single-bundle PCL reconstruction using standard anterior and posteromedial portal with remnant preservation technique. We hypothesized that PCL reconstruction using standard anterior and posteromedial portal with remnant preservation technique provides good clinical outcomes.
2. MATERIALS AND METHODS
This study was a cohort retrospective study at Soeradji Tirtonegoro General Hospital from January 2013 to December 2015. It was reviewed and approved by the Medical and Health Research Ethics Committee at the Faculty of Medicine of Gadjah Mada University. Informed consent was obtained from all patients.
PCL rupture was diagnosed using clinical examination (posterior sagging sign, posterior drawer test grade 3) and Magnetic Resonance Imaging (MRI) that indicates grade 3 PCL rupture. PCL reconstruction was performed on patients with grade 3 PCL rupture (posterior drawer examination ≥11 mm side-to-side difference in posterior displacement), who still complained of pain and instability in their knee despite conservative treatment for at least 3 months.
The exclusion criteria were patients with other ligament injury and associated fractures in the lower extremity.
2.1. Surgical Technique
A single senior knee surgeon performed all procedures. Patients lay in supine position under regional anesthesia, the tourniquet was applied in the thigh and inflated without elevation and exsanguination. Standard anterolateral and anteromedial portals were used. Diagnostic arthroscopy was performed, followed by hamstring graft harvesting.
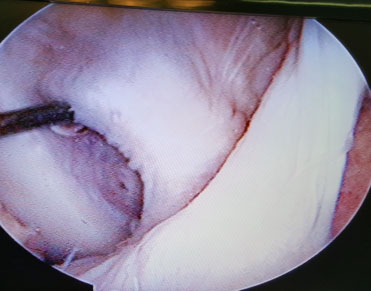
Synovial and fat-like tissue on the femoral attachment of the PCL remnant were removed carefully to expose the fibers of PCL bundles. The PCL remnants were preserved (Fig. 1). The femoral tunnel was placed at 8 to 10 mm from the anterior or distal medial femoral articular margin on a continuous line with the junction of the roof and medial wall of the intercondylar notch. A 2.0 mm Kirschner wire was inserted through the reamer to serve as a guidewire. Over drilling was done with a 5 mm diameter drill (ConMed-Linvatec; USA) using the anterolateral portal. A 2.4-mm pin was passed through the femoral tunnel and reamed using the cannulated drill in accordance with graft diameter at the distal portion until 30 mm depth of the femoral tunnel.
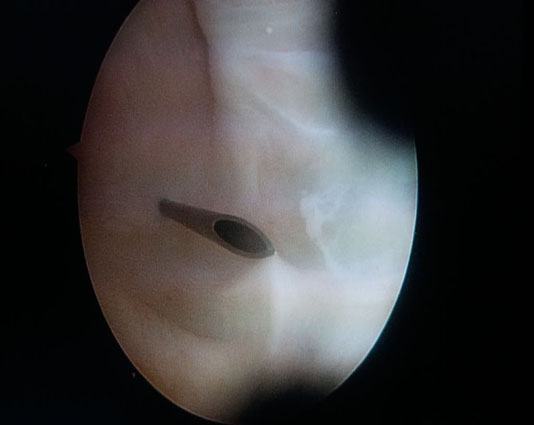
A posteromedial portal was created under direct vision (Fig. 2). The PCL tibial attachment site was completely exposed. A guide pin was inserted through the anteromedial incision within the distal center portion of the tibial insertion of PCL, which comes into contact with the posterior edge of the retrospinal surface. The tibial hole was made in accordance with graft diameter. A 2.4-mm (blunt leading end) pin was inserted through this hole. A pullout suture was threaded in a retrograde fashion. Using this, the 4-strand hamstring graft was pulled through the femoral hole. Proximal femoral fixation was obtained using Graftmax button® (ConMed-Linvatec; Utica, NewYork, USA). Button was flipped outside the medial cortex of the femur. Then, the graft was grasped and pulled tightly out of the anterior tibial hole, and a 25-35 mm BioScrew® (ConMed-Linvatec; Utica, NewYork, USA) was inserted at 90° knee flexion maintained with anterior drawer.
2.2. Postoperative Rehabilitation
The knee was immobilized for 4 weeks with a brace in extension. Ambulation with non-weight bearing was initiated on the second postoperative day. Quadriceps isometric exercise and straight-leg raising exercise should be initiated after 2 weeks. Protected ROM was gradually increased from 0-90° flexion starting from the fourth to eighth week. After 8 weeks, knee flexion from 90° - full ROM was exercised gradually. Partial weight-bearing was permitted after 4 weeks. Full weight -bearing with hamstring-strengthening exercises was permitted after 8 weeks and active knee ROM should progress to complete flexion and extension. Patients usually returned to their normal daily activity and were allowed to exercise on a stationary bike or standing on a single leg starting at 5 months postoperatively. Light sports activities began at 6 months. After 12 months, the patient will be tested with a serial hop test then cleared for sport activities.
2.3. Clinical and Functional Evaluation
Functional evaluation was performed preoperatively and 24 months after surgery using International Knee Documentation Committee (IKDC), Knee Society Score, Lysholm knee score, and Modified Cincinnati Score. A single physician did the interviews. Ligament testing was performed using the posterior drawer test. The complication was evaluated post-operatively 24 months after surgery.
2.4. Statistical Analysis
Wilcoxon signed rank test was used for IKDC, KSS, Lysholm knee score, and Modified Cincinnati score. The value of p < 0.005 was regarded as significant. All of the statistical analysis was done using SPSS version 25 for Windows® using dependent t-test p<0.05.
3. RESULTS
There were 25 patients who met the inclusion criteria. They consisted of 10 males and 15 females with a mean age of 28.36±11.67 (16-57) years old. Injury mechanism obtained 5 patients at sports, 1 patient after forced hyperextension of the knee, and 19 patients from traffic accidents. The site of PCL injury was described 15 in the right knee and 10 in the left knee. The demographic data are shown in Table 1.
Knee functional score showed improvement score at 2-years postoperative based on Lysholm Knee Score, IKDC, Modified Cincinnati Score, and Knee Function Score, as shown in Table 2. ROM evaluation showed that 22 patients (79%) achieved normal ROM at final follow up and three patients (21%) had ROM restriction (0-110°).
| Variable | Result |
|---|---|
| Age | 28.36±11.67 (17 – 56) |
| Gender | Male: 10. Female:15 |
| Mechanism of Injury | MVA:19, sports:5, others:1 |
| Site of injury | Right: 15, Left: 10 |
| – | Mean | Mean difference | 95% CI | p value |
|---|---|---|---|---|
| Lysholm Knee Score | – | – | – | – |
| Pre-operatve | 65.12±10.48 | -29.84±11.47 | (-34.57) – (-25.10) | <0.001 |
| 2-years Follow-up | 94.96±4.80 | |||
| IKDC | – | – | – | – |
| Pre-operatve | 60.50±15.10 | -35.10±15.19 | (-41.37) – (-28.83) | <0.001 |
| 2-years Follow-up | 95.60±3.44 | |||
| Modified Cincinnati Score | – | – | – | – |
| Pre-operatve | 62.28±13.63 | -33.76±13.67 | (-39.40) – (-28.11) | <0.001 |
| 2-years Follow-up | 96.04±1.62 | |||
| Knee Society Score | – | – | – | – |
| Pre-operatve | 60.16±18.01 | -34.72±16.72 | (-41.62) – (-27.81) | <0.001 |
| 2-years Follow-up | 94.88±6.36 |
There was no numbness at the medial knee in any patient. No deep infection, thrombophlebitis, or vascular injury was noted in this study. Two patients (14%) developed surgical site infection in the tibial site 1 month after surgery, which was successfully treated with local debridement.
4. DISCUSSION
Isolated rupture of the PCL stands for a distinctive subgroup of traumatic injuries of the knee. PCL injury is reported between 3% to 37% of all knee ligament injuries [11, 12]. Despite that most PCL injury may be treated conservatively, in some patients, symptoms such as pain during exercise and inability to run due to the pain itself still occurs. The challenges in the management of PCL injury are related to the single or double bundle techniques, graft selection, tunnel placement, fixation, and either remnant preservation or non-preservation technique [13]. Nevertheless, there is no single PCL reconstruction technique that is accepted widely. This study suggested that arthroscopic PCL reconstruction using standard anterior and posteromedial portal with remnant preservation improves functional outcome significantly than PCL deficient patients who had failed conservative management.
Clear visualization and exposure of the origin of the PCL are critical for the safety and success of the PCL reconstruction procedure. The insertion of the PCL on the posterior tibial upslope can be clearly visualized surgically at the time of reconstruction by having an appropriate amount of soft tissue and PCL remnant debridement. Various techniques such as utilization of a 70° arthroscope, posterolateral portal approach, a midline trans-patellar tendon approach, or a posterior trans-septal portal approach technique have been shown from previous studies to have a better visualization of the retained PCL remnant [5, 6, 10, 14-16]. However, there are potential surgery associated morbidities related to additional portals techniques as well as the implementation of variable angle arthroscopic techniques. Additional surgery time was also affected by these techniques.
A number of techniques to visualize the posterior compartment were proven to be safe. These techniques were posteromedial portal, posterolateral portal, and anterior portal technique. In anterior portal technique, arthroscope was introduced through anterior portals into the posterior compartment across the intercondylar notch. This approach will give a good visualization of the posterior compartment. In order to create posterior trans-septal portal, it is necessary to have the trans-notch approach of the arthroscope or instruments. Nevertheless, in knees that are small or knees with prominent spurs around the tibial spine, the transnotch approach may be difficult. For about 34% of the arthroscopies, it may be difficult to explore the posterior compartment adequately from an anterior portal. These were related to several factors, including intercondylar notch mechanical blockage, inexperienced surgeon, and degenerative joint disease cases. The failure of the triangulation of the arthroscope and the instrument has been acknowledged by many arthroscopic surgeons to be the cause of unsuccessful arthroscopic procedures in certain areas of the posterior compartment [5, 6, 10, 14-16]. Previous studies stated that PCL reconstruction with PCL remnant preservation gave good healing capacity and possible proprioception [10, 17].
In this study, we used only posteromedial portal to achieve clear visualization, with the preservation of PCL remnant. This procedure is safer with 70º arthroscope or additional instrument. This technique is simpler especially for junior surgeons and requires shorter surgical time because it does not need posterolateral portal or additional instrument.
The common risk in the posteromedial portal approach is complications related to the saphenous nerve and vein [15]. In a study by McGinnis et al., a spot in the knee, the so-called “anatomical soft spot” is a safe area to locate the posteromedial portal [18]. It is surrounded by the posterior edge of the medial condyle of the femur, hamstrings, and medial tibial plateau. Following the posteromedial portal, it can be made safer by positioning the knee in 90º flexion than in an extended position. The former position will move the saphenous nerve and vessels more posteriorly than the latter position. The mean distance between the posteromedial portal location and the saphenous nerve is around 22-26 mm at a 90 º flexion [18].
The preservation of PCL remnant augmentation was recently proposed as a technique for PCL reconstruction. It has the ability to achieve an isometric and anatomic position of the PCL graft, even though it is technically difficult. In the past, it was necessary to remove the remnant and footprints of PCL for fine visualization of tunnel placement. However, many authors have recently proposed the concept of preservation of PCL remnant, which can increase the length of the PCL graft and allow more anatomic positions [10, 19]. A study by Jae Ang sim et al. compared the clinical and radiological results between posteromedial and posterior trans-septal portal technique. It showed that there were no significant differences in clinical results for both groups in creating tibial tunnel of single bundle PCL reconstruction with remnant preservation technique [20].
In our study, all patients were assessed by means of IKDC (International Knee Documentation Committee) subjective knee score, Lysholm knee score, Modified Cincinnati Score, and KSS (Knee Society Score) pre-operative and 2 years post-operative. IKDC and Lysholm knee assessment systems have been used extensively to analyze the results of PCL reconstruction. Both the IKDC and Lysholm knee assessment systems are fairly reliable methods to assess knee function.
Evaluation of the IKDC score combined between signs and symptoms of knee function. The subjective evaluation of IKDC is based on self-assessments reported by patients regarding their function and level of knee activity. This study showed that there was an improvement in the IKDC score from an average number of 60 to 95 after 2 years of follow-up in PCL reconstruction patients. The average of Lysholm rating system score increased from 66 presurgery to 94 at 2-years follow-up post-surgery. The Modified Cincinnati Score system is designed to provide information about how knee pain affects the patient's ability to manage daily life activities. The average Modified Cincinnati score increased from 62 pre-operative to 96 at 2-years follow-up. This score related to the intensity of pain, swelling, and overall activity levels such as walking, running, going up and down the stairs, and jumping. Meanwhile, the Knee Society Score increased from 60 before surgery to 94 at 2-years follow-up. The variables of this assessment include pain, total range of flexion and extension, instability, walking activity, up and down the stairs with walker.
We believe that this study is unique for a number of reasons. PCL reconstruction using posteromedial portal is a simpler and safer technique. In addition, it can give a good visualization of PCL tibial footprint with preserved PCL remnants. However, the limitations of the work must be acknowledged. First, there was no control group in this study. However, this study had minimized the bias by using a single surgeon and a single physician to interview all patients. Secondly, this study only evaluated mid-term follow-up. Long-term follow-up is needed to evaluate further about this technique. Thirdly, this study did not evaluate proprioceptive function, joint laxity, and graft healing with preserved remnant, which was the most considered reason for remnant preservation technique. We also hope the next future study will compare the usage of posteromedial portal and other portals to develop the best technique in PCL reconstruction.
CONCLUSION
In conclusion, the clinical and functional outcomes in patients post PCL reconstruction using standard anterior and posteromedial portal with remnant preservation have significant improvement based on the IKDC score, KSS, Lysholm Knee Scoring Scale, Modified Cincinnati Score at 2 years follow-up.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
It was reviewed and approved by the Medical and Health Research Ethics Committee at the Faculty of Medicine of Gadjah Mada University, Indonesia.
HUMAN AND ANIMAL RIGHTS
Not applicable.
CONSENT FOR PUBLICATION
Informed consent was obtained from all patients.
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


